Skin cancer is the most common of all cancer types in Canada, accounting for an estimated one-third of new cancer cases diagnosed each year.
Skin cancer can be classified as melanoma and non-melanoma – non-melanoma skin cancer (NMSC) can also be further separated as basal cell carcinoma (BCC) and squamous cell carcinoma (SCC) based on the type of cell in which the cancer originates. Melanoma is a cancer that develops in the skin’s melanocytes, or the skin cells located near the bottom layer of the epidermis that produce melanin.
Most skin cancers detected in Canada are non-melanoma and typically occur on areas that receive frequent sun exposure, including the face, neck, and hands. Melanoma accounts for approximately 5 percent of skin cancer diagnoses and can develop almost anywhere on the body, even in areas that receive little to no sun.
As incident rates of both melanoma and non-melanoma skin cancers rise, so do mortality rates, with numbers increasing five-fold in some provinces in recent years.
It’s now estimated that 1 in 42 men and 1 in 56 women will develop melanoma during their lifetime, and 1 in 219 men and 1 in 402 women will die of it.
Early detection is key – when caught early, melanoma can be treated successfully with survival rates between 40-97 percent, however once metastasis occurs, survival rates drop substantially to 15-20 percent.
Family physicians are often the first line of defense in detecting skin cancer – ensuring you and your patients know what to look for can save lives.
Risk factors for developing skin cancer
Though there is no single cause of skin cancer, approximately 90 percent of skin cancers are caused by UV rays. Other factors that enhance risk include:
- Personal or family history of melanoma
- Severe, blistering sunburns before the age of 20
- Presence of moles – especially if there are many, or if they are unusual or large
- Sun sensitivity – skin that is easily burnt or difficult to tan
- Light coloured skin, eyes, and hair
- History of excessive sun exposure
- Diseases that suppress the immune system
- Exposure to UV radiation including tanning beds and sun lamps
What to look for
Checking your skin often for changes and new lumps, bumps or growths is critical to catching skin cancer early when it’s easier to treat. Though not all skin cancers will look like the examples below, the following are general guidelines on what to look for.
Basal cell carcinoma
Most BCC initially appear as a small ‘pearly’ bump similar to a flesh-coloured mole or pimple that does not go away. Growths can also appear dark in colour, or as pink patches with scaling or a slightly shiny appearance. They can also appear as hard, scar-like growths.
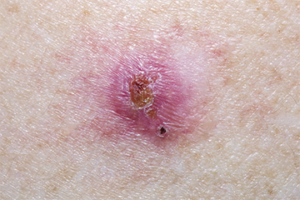
Squamous cell carcinoma
Most incidents of SCC are caused by sun exposure or sun damage. In early stages, SCC can appear as small, skin-coloured or red nodules, usually with a rough surface. They can also resemble warts or bruises with raised, crusty edges. Lesions develop slowly, but over time, can grow into a large tumor. Crusting, ulceration, and bleeding might occur.
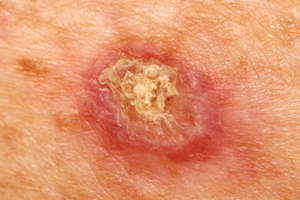
Melanoma
The first sign of melanoma is typically a change in the shape, colour, size, or feel of an existing mole, however it may also appear as a new mole. Melanoma occurs most frequently on the legs for women, and on the chest or back for men, however they can be found on the face and neck and in areas not typically exposed to the sun.
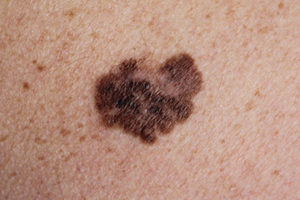
The ABCDEs and the Ugly Duckling methods are both frequently used to detect melanoma.
ABCDE method
When checking moles, look for:
Asymmetry. Most melanomas are asymmetrical – if you draw a line through the middle of the lesion, the two halves would not look the same.
Border. Melanoma borders tend to be uneven and may have scalloped or notched edges.
Colour.Normal moles are usually a single shade of brown. A melanoma may have multiple colours, including different shades of brown, tan or black. As it grows, white, red or blue may also develop.
Diameter. Look for lesions the size of a pencil eraser (6mm) and larger.
Evolving. Look for any changes in size, shape, colour or elevation of a spot on your skin, or any new symptoms such as bleeding, itching or crusting.
Ugly duckling method
Ugly duckling lesions are moles or spots that look different from surrounding moles. They will typically appear larger, smaller, lighter, or darker than their neighbours.
How can you protect yourself?
The best way to lower your risk of developing skin cancer is to be sun smart.
- Avoid sun exposure during the middle of the day when the sun’s rays are strongest
- Wear sunscreen (SPF 30 or higher) year-round
- Wear protective clothing (long-sleeve shirts, hats, sunglasses)
- Avoid tanning beds
- Check your body often for changes in existing moles or the appearance of new moles. If you have any doubts, talk to your family doctor or dermatologist immediately.
+ + +
Clinicians: Stay current on the latest skin cancer diagnosis and treatments. This complimentary course from MDBriefCase will improve your ability to:
- Recognize and clinically diagnose skin cancers.
- Select which biopsy would be appropriate to perform on a suspicious skin lesion.
- Describe the available treatment options for different types of skin cancer.
- Apply knowledge to enable earlier diagnosis and management of patients with skin cancer.
