2023-07-20
Hepatitis Vaccination: Myths, Facts, and Strategies To Overcome Vaccine Hesitancy
Share:
MDBriefCase will be unavailable due to maintenance from Sunday, January 14 11PM to Monday, January 15 1AM ET.
Welcome
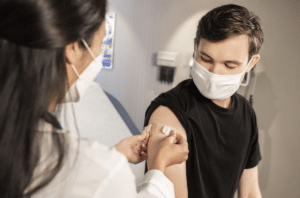
Infection with hepatitis C virus is a global public health concern. A recent study found that Canada is on track to achieve hepatitis C elimination goals set by the World Health Organization if treatment levels are maintained, however, many provinces began to see a decrease in vaccinations prior to the COVID-19 pandemic.
Hepatitis viruses easily spread to others, causing liver infections and damage. Vaccines can protect against some hepatitis viruses, but patients may worry about myths concerning side effects and risks.
Fact: Hepatitis vaccines do not contain live viruses and cannot cause hepatitis.
Hepatitis vaccines are made with inactivated viruses or surface proteins. These components teach the immune system to recognize hepatitis and trigger an immune response, protecting against future infections.
There are several approved vaccine products available. The hepatitis A vaccines use inactivated or dead viruses incapable of infecting cells.
The hepatitis B vaccines contain viral proteins, known as recombinant vaccines. Scientists isolate a section of the gene in the hepatitis B virus that makes the surface proteins and insert these genes into a yeast cell. These yeast cells then make these surface proteins, which are harvested and used in vaccines but are also incapable of infecting cells.
Fact: Hepatitis B vaccines do not cause multiple sclerosis (MS) or trigger MS flare-ups.
The fear that hepatitis B vaccines cause MS dates back to a 1998 study that reported a link between the vaccine and a nerve disease known as MS. Several studies have been completed since then and found no association between hepatitis B vaccines and the development of MS in children or adults.
Millions of people have received hepatitis vaccines, yet don’t have MS. Additionally, Health Canada reviews, approves, and monitors all vaccines for use in the public. Vaccine manufacturers must prove that vaccines work, are safe to use, and are manufactured under strict quality control.
Fact: Hepatitis infections can and do happen in unexpected ways.
Hepatitis A infections, for example, spread through contact with infected stool. You can get hepatitis A when you eat or drink food and water contaminated with infected stool. Some Canadians are more likely to get hepatitis A, including:
Hepatitis B, on the other hand, is spread through contact with infected bodily fluids. You can contract hepatitis B from:
Healthcare workers or other people who handle blood can also become infected with the virus. Mothers can also spread hepatitis B to babies during birth.
Vaccine hesitancy is common, especially among parents. Recent data shows that only 3 percent of parents refuse vaccines outright, but 19 percent describe themselves as hesitant.
While research on vaccine hesitancy is limited, a review study shows that a few key strategies work best to overcome hesitation. Healthcare workers should:
Hepatitis vaccines are essential tools that promote health and prevent infectious diseases. MDBriefCase offers accredited courses to help you stay up-to-date on current research and strategies. Join for free today.
In submitting your work (the “Work”) for potential posting on the MDBriefCase Healthcare Leadership Academy website (the “Website”), you (“You”) expressly agree to the following:
Review: MDBriefCase is pleased to consider the publication of Your Work on the Website. The suitability of the Work for posting shall be determined by MDBRiefCase at its sole discretion. Nothing herein shall obligate MDBriefcase to post or otherwise publish the Work, or the maintain its posting in future.
Editing; Identification: MDBriefcase shall have the right to edit the Work to conform to our standards of style, technological requirements, language usage, grammar and punctuation, provided that the meaning of the Work is not materially altered. If posted, You will be identified as the author of the Work, or co-author if applicable.
Grant of Rights: As a condition of publication and for no monetary compensation, You hereby grant to MDBriefCase the following rights to the Work in any and all media whether now existing or hereafter developed, including print and electronic/digital formats: (1) the exclusive right of first publication worldwide; (2) the perpetual non-exclusive worldwide right to publish, reproduce, distribute, sell, adapt, perform, display, sublicense, and create derivative works, alone or in conjunction with other materials; (3) the perpetual non-exclusive worldwide right to use the Work, or any part thereof, in any other publication produced by MDBriefCase and/or on MDBriefCase’s website; and (4) the perpetual non-exclusive worldwide right to use the Work to promote and publicize MDBriefCase or its publications. The grant of rights survives termination or expiration of this Agreement.
Warranty: You warrant that the Work is original with You and that it is not subject to any third party copyright; that You have authority to grant the rights in this Agreement; that publication of the Work will not libel anyone or infringe on or invade the rights of others; that You have full power and authority to enter into this Agreement; that the Work has not been published elsewhere in whole or in part; and that You have obtained permission from the copyright owner consistent with this Agreement for any third party copyrighted material in the Work. This warranty survives termination or expiration of this Agreement.
Thank you for your interest in writing an article for the MDBriefCase Healthcare Leadership Academy website.
The Healthcare Leadership Academy welcomes submissions on all topics relevant to leaders in healthcare. Our topics include Leading in Healthcare, Leadership Lessons from COVID-19 and others. We prioritize stories that provide leadership advice to executives and managers in healthcare companies, offer actionable strategies for executing successful projects, and provide interesting angles on current healthcare topics. Submissions must be original work of the authors and unpublished. When submitting, authors represent that they have included no material that is in violation of the rights of any other person or entity.
Articles must be educational and non-promotional. If they mention the author’s company or any of the company’s products or services by name within the text, such mention should be very limited and used for reference only, not for promotion. (For example, an author might cite a survey conducted by his company but not describe his company’s product as a solution to a business problem.) Articles will be edited for clarity, style and brevity. The final headline is determined by the editor.
Guest articles for the MDBriefCase Healthcare Leadership Academy may run between 500 and 1000 words.
MDBriefCase reserves the right to accept or reject any submission and the right to condition acceptance upon revision of material to conform to its criteria.
There is no payment for contributed articles. However, MDBriefCase will give the author a byline. Authors are invited to link to the article on personal websites, corporate websites and social media platforms.
Each author understands and agrees that any submission accepted for posting is provided subject to MDBriefCase’s Author Agreement.
This website uses cookies so that we can provide you with the best user experience possible. Cookie information is stored in your browser and performs functions such as recognising you when you return to our website and helping our team to understand which sections of the website you find most interesting and useful.
Strictly Necessary Cookie should be enabled at all times so that we can save your preferences for cookie settings.
If you disable this cookie, we will not be able to save your preferences. This means that every time you visit this website you will need to enable or disable cookies again.
This website uses Google Analytics and other tools to collect anonymous information such as the number of visitors to the site, and the most popular pages. Additional information may be collected for analysis.
Keeping this cookie enabled helps us to improve our website.
Please enable Strictly Necessary Cookies first so that we can save your preferences!